The emergency room (ER) is the front line of healthcare, providing immediate care to patients facing life-threatening conditions or sudden illnesses. For many, visiting the ER can be stressful and confusing, especially if they are unfamiliar with how emergency care operates. Understanding emergency room protocols can help patients navigate the system effectively, ensure timely treatment, and improve outcomes. ER protocols encompass everything from triage and patient registration to treatment prioritization and discharge procedures. Modern ERs combine medical expertise, technology, and streamlined processes to handle emergencies efficiently.
What Are Emergency Room Protocols?
Emergency room protocols are standardized procedures and guidelines followed by healthcare providers to deliver immediate, effective, and organized care to patients in urgent situations. These protocols are designed to prioritize patients based on the severity of their condition, ensure proper documentation, and facilitate communication between medical staff. They help minimize errors, improve patient outcomes, and maintain safety in high-pressure situations.
Key Objectives of ER Protocols
- Rapid Assessment: Quickly identify life-threatening conditions.
- Prioritization of Care: Triage patients based on severity and urgency.
- Efficient Treatment: Ensure timely administration of medication, interventions, or procedures.
- Documentation: Maintain accurate medical records for continuity of care and legal compliance.
- Patient Safety: Reduce risks, prevent errors, and manage infectious diseases effectively.
The Triage Process
Triage is the first step in the emergency room and determines the order in which patients receive care. The goal is to ensure that the most critically ill or injured patients are treated first.
Levels of Triage
- Level 1 – Immediate: Life-threatening conditions requiring urgent intervention, such as cardiac arrest, severe trauma, or respiratory failure.
- Level 2 – Emergent: Serious conditions that need rapid attention but are not immediately life-threatening, such as severe asthma attacks or major fractures.
- Level 3 – Urgent: Conditions that require prompt care but can safely wait for a short period, like minor head injuries or moderate infections.
- Level 4 – Semi-Urgent: Non-life-threatening conditions that need medical attention but can wait longer, such as sprains or mild abdominal pain.
- Level 5 – Non-Urgent: Minor ailments like colds, minor cuts, or mild fever that could be treated in a primary care setting.
Triage Assessment Factors
- Vital signs (blood pressure, heart rate, oxygen levels)
- Presenting symptoms and severity
- Age and medical history
- Risk of deterioration
Patient Registration and Documentation
After triage, patients are registered in the hospital system. Accurate documentation is critical for medical, legal, and insurance purposes. Registration involves collecting personal details, medical history, allergies, and insurance information. Modern ERs often use electronic health records (EHRs) to streamline documentation and ensure information is accessible to the medical team in real time.
Importance of Documentation
- Tracks patient care and interventions
- Facilitates communication between healthcare providers
- Supports insurance claims and legal compliance
- Ensures continuity of care for follow-up treatment
Initial Assessment and Stabilization
Once registered, patients undergo a primary assessment, often referred to as the primary survey, to stabilize vital functions. The primary survey follows the ABCDE approach:
- A – Airway: Ensure the patient’s airway is open and unobstructed.
- B – Breathing: Assess breathing and provide oxygen or ventilation if necessary.
- C – Circulation: Check pulse, blood pressure, and signs of shock; provide IV fluids or medications.
- D – Disability: Evaluate neurological status, level of consciousness, and responsiveness.
- E – Exposure: Examine for injuries or underlying conditions while maintaining body temperature.
Emergency Interventions
- Cardiac monitoring and defibrillation for heart emergencies
- Administration of emergency medications (epinephrine, pain relief, antibiotics)
- Wound care, fracture stabilization, or surgical intervention as needed
- Respiratory support using oxygen therapy, nebulizers, or intubation
Diagnostic Tests in the ER
Prompt diagnosis is critical in emergency care. ER protocols include ordering and interpreting essential diagnostic tests quickly.
Common Tests
- Blood Tests: Complete blood count, electrolytes, cardiac markers
- Imaging: X-rays, CT scans, MRI, and ultrasound to detect injuries or internal conditions
- Electrocardiogram (ECG): Monitors heart activity in suspected cardiac cases
- Urinalysis: Detects infections or kidney issues
- Rapid Tests: Blood sugar, infectious disease screenings, and pregnancy tests
Treatment Protocols
Treatment in the ER is guided by the patient’s condition, test results, and severity of illness. Protocols ensure evidence-based care, reduce errors, and optimize outcomes.
Medication Administration
Medications may include pain relievers, antibiotics, antivirals, anticoagulants, or emergency drugs like epinephrine or nitroglycerin. Proper dosing and monitoring are essential, especially in pediatric, geriatric, or critical patients.
Procedures and Interventions
- Minor procedures: Suturing, wound cleaning, splinting fractures
- Major procedures: Emergency surgery, chest tube insertion, or resuscitation
- Specialized interventions: Cardiac catheterization, endoscopy, or airway management
Patient Monitoring
Continuous monitoring of vitals, oxygen levels, cardiac function, and neurological status is standard. ER nurses and technicians are trained to recognize early signs of deterioration and escalate care promptly.
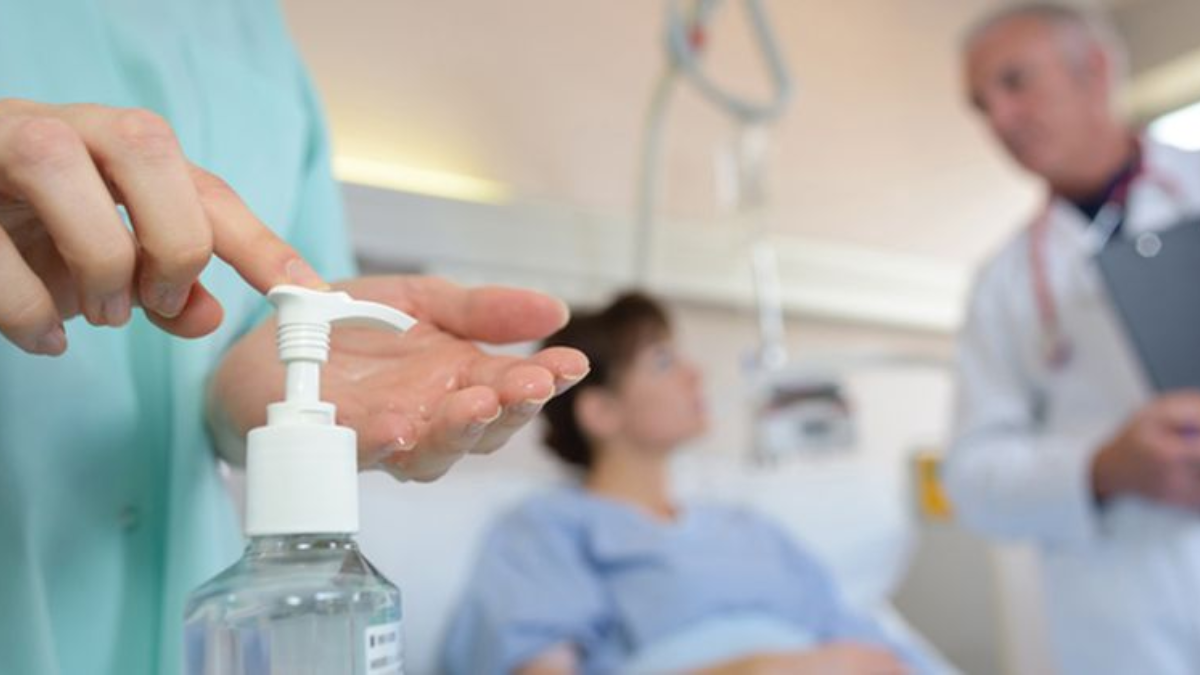
Infection Control in the ER
Emergency rooms handle patients with a variety of infectious conditions. Strict infection control protocols are essential to prevent the spread of disease.
- Hand hygiene and use of personal protective equipment (PPE)
- Isolation rooms for contagious patients
- Sterilization of medical equipment and surfaces
- Waste disposal protocols for biohazard materials
Communication and Coordination
Effective communication between ER staff, specialists, and other hospital departments is crucial. Protocols include standardized handovers, electronic alerts, and clear documentation to ensure continuity of care.
Multidisciplinary Teams
ER care often involves a team of physicians, nurses, technicians, pharmacists, and social workers. Team-based protocols ensure that all aspects of patient care are coordinated efficiently.
Discharge and Follow-Up
Once stabilized, patients may be discharged, admitted to the hospital, or transferred to another facility. Discharge protocols include:
- Providing instructions for medications, wound care, or lifestyle adjustments
- Scheduling follow-up appointments
- Offering information on warning signs that require immediate return to the ER
- Coordinating with primary care physicians or specialists
Patient Education
Educating patients and caregivers on post-ER care is essential to prevent complications, reduce readmissions, and support recovery.
Common Challenges in ER Management
Emergency rooms face unique challenges due to high patient volumes and unpredictable cases.
Overcrowding
ERs often experience overcrowding, leading to longer wait times and strained resources. Efficient triage and resource allocation help mitigate this issue.
Staff Burnout
The high-stress environment, long shifts, and exposure to critical situations can lead to burnout among healthcare professionals.
Medical Errors
Errors in medication, diagnosis, or procedures can occur in fast-paced ER settings. Protocols, checklists, and double-check systems reduce risks.
Resource Limitations
Availability of beds, medical equipment, and specialized staff can impact timely care, especially during emergencies or pandemics.
The Role of Technology in ER Protocols
Technology has transformed emergency care, making it faster, more accurate, and more efficient.
Electronic Health Records
EHRs provide real-time access to patient history, allergies, and medications, enabling informed decision-making and reducing errors.
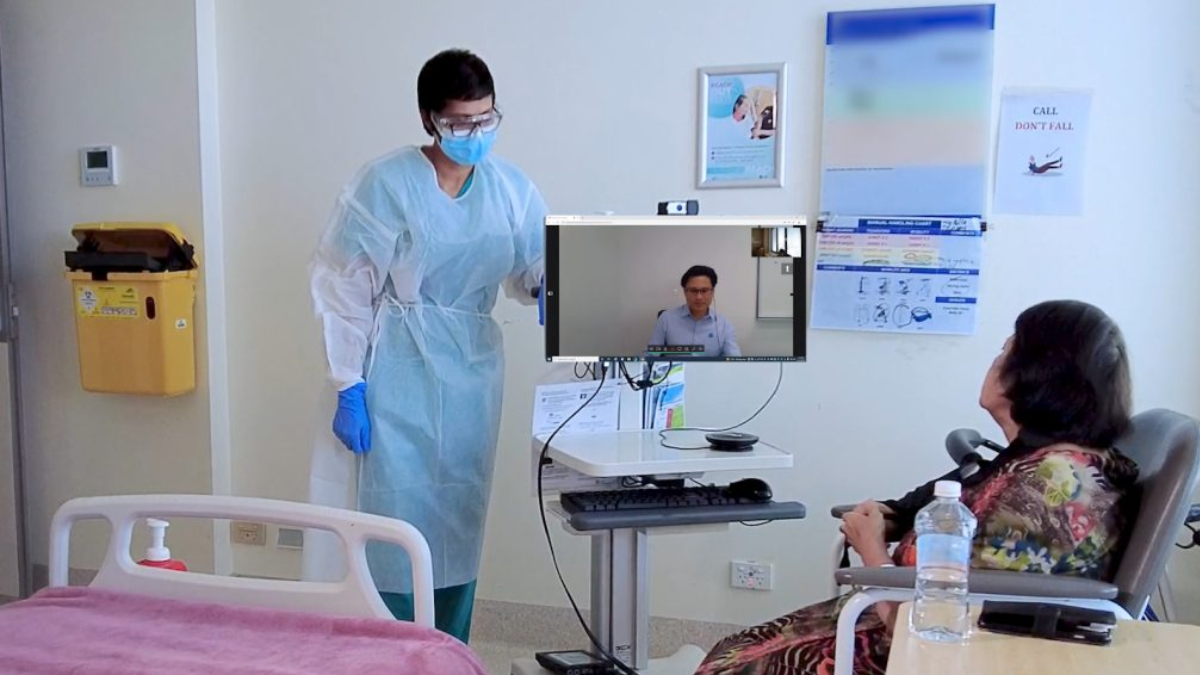
Telemedicine
Tele-ER consultations allow remote evaluation and guidance from specialists, especially in rural or underserved areas.
AI and Predictive Analytics
AI algorithms help predict patient deterioration, identify high-risk cases, and optimize resource allocation in the ER.
Automated Monitoring Systems
Smart devices continuously monitor vital signs, alerting staff to critical changes instantly.
Conclusion
Emergency room protocols are essential for delivering organized, efficient, and life-saving care. From triage and patient assessment to diagnostic testing, treatment, and discharge, ER protocols ensure that patients receive timely and appropriate care in high-pressure situations. By understanding how ERs operate, patients can navigate the system more effectively, follow instructions accurately, and advocate for themselves or their loved ones. The integration of technology, standardized procedures, and multidisciplinary teamwork continues to improve the quality, safety, and outcomes of emergency care, making ERs a cornerstone of modern healthcare.
FAQs
1. What is the first step when entering an emergency room?
The first step is triage, where medical staff assess the severity of your condition and prioritize care based on urgency.
2. How are patients prioritized in the ER?
Patients are prioritized using a triage system that categorizes conditions from life-threatening to non-urgent based on symptoms and vital signs.
3. Can anyone visit the ER without an appointment?
Yes, emergency rooms are open to anyone in need of urgent or life-threatening care, regardless of appointment or insurance status.
4. How long will I have to wait in the ER?
Wait times vary depending on the severity of your condition and the ER’s patient volume; critical cases are treated immediately.
5. What should I bring to the ER?
Bring identification, insurance information, a list of medications, medical history, and any relevant documents to assist with registration and treatment.