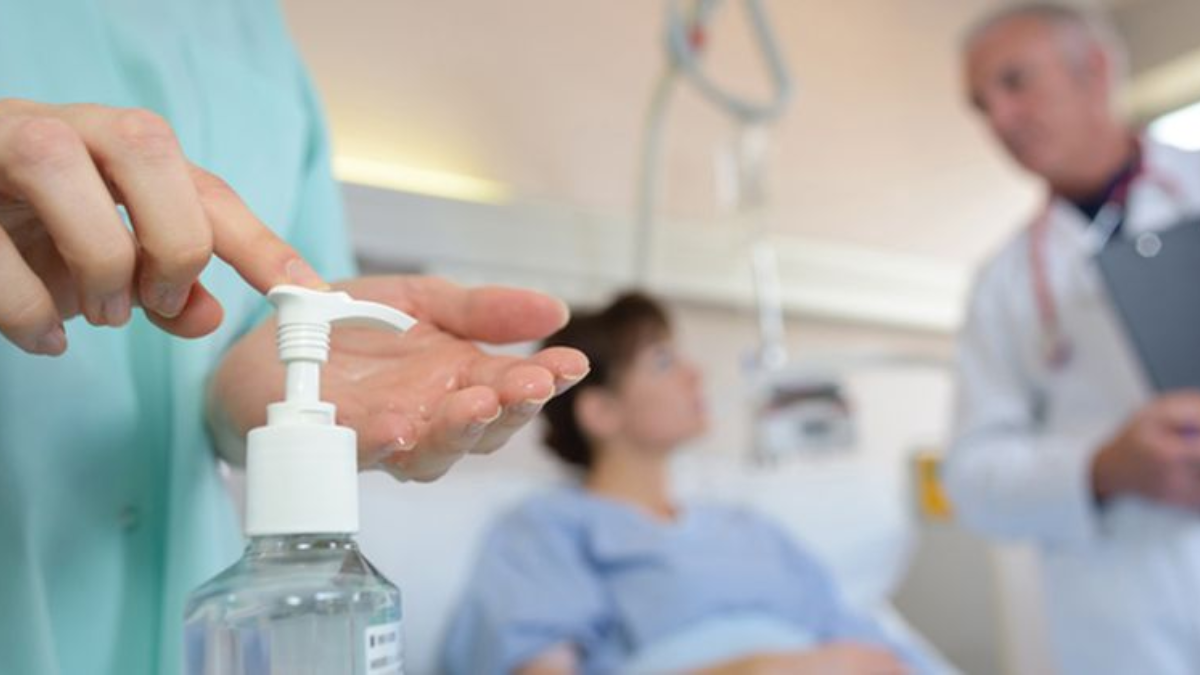
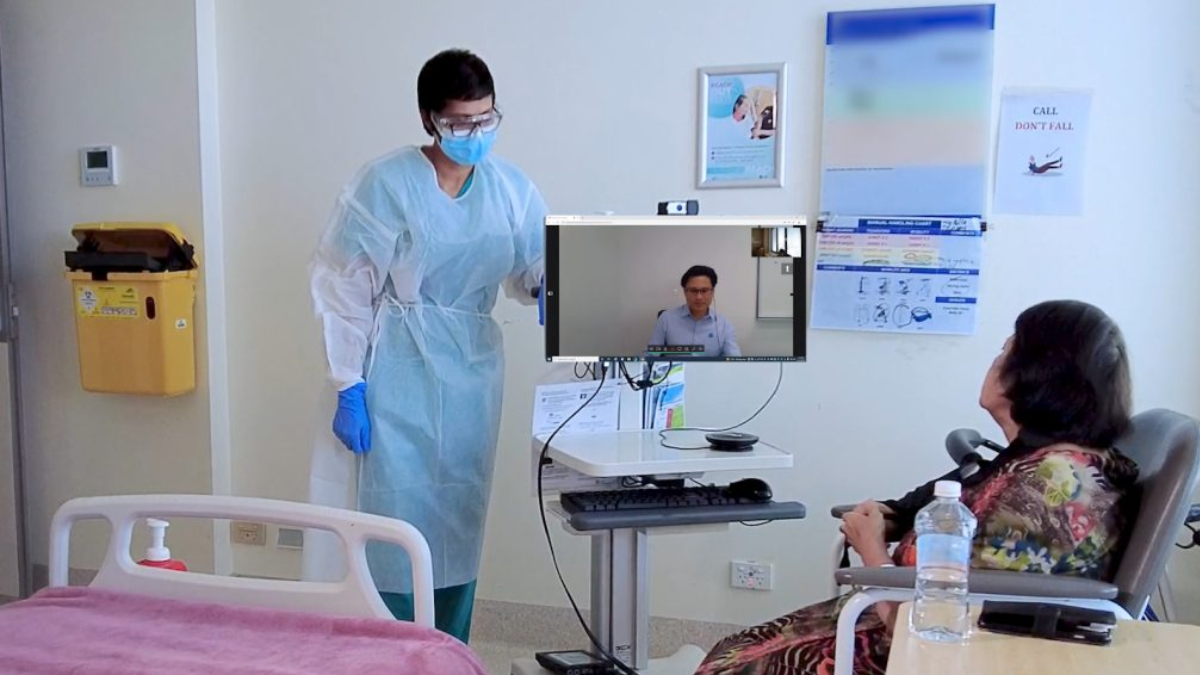
Hospital hygiene and sanitation are fundamental aspects of healthcare that ensure patient safety, prevent infections, and promote overall well-being. Maintaining a clean and sterile environment in hospitals is critical due to the high risk of healthcare-associated infections (HAIs) that can compromise patient outcomes. Hospitals must adopt rigorous hygiene and sanitation protocols, including hand hygiene, sterilization of equipment, environmental cleaning, and waste management. This article explores best practices for hospital hygiene and sanitation, their importance, and how they contribute to patient safety.
Importance of Hospital Hygiene and Sanitation
Proper hygiene and sanitation in hospitals are essential for several reasons:
- Prevention of Infections: Reduces the risk of HAIs such as MRSA, C. difficile, and surgical site infections.
- Patient Safety: Ensures a safe environment for vulnerable patients, including those with weakened immune systems.
- Compliance with Regulations: Hospitals must adhere to guidelines from bodies like the CDC, WHO, and local health authorities.
- Public Trust: Clean hospitals enhance patient confidence and institutional reputation.
- Operational Efficiency: Reduces patient complications, hospital stay durations, and associated healthcare costs.
Key Areas of Hospital Hygiene
Hospital hygiene encompasses multiple domains, from personal hygiene of staff to environmental sanitation.
Hand Hygiene
Hand hygiene is the single most important measure to prevent infection transmission.
- Handwashing: Use of soap and water for at least 20 seconds.
- Alcohol-Based Sanitizers: Effective for most pathogens when hands are not visibly soiled.
- Compliance Monitoring: Hospitals should enforce hand hygiene protocols for staff, patients, and visitors.
Personal Protective Equipment (PPE)
PPE prevents the spread of infectious agents.
- Gloves, Masks, and Gowns: Worn appropriately based on patient risk and procedures.
- Eye Protection: Shields against splashes and droplets.
- Proper Disposal: Used PPE must be disposed of following biohazard protocols.
Environmental Cleaning
Cleaning and disinfecting hospital surfaces prevent the persistence of pathogens.
- High-Touch Surfaces: Regular disinfection of door handles, bed rails, switches, and medical equipment.
- Patient Rooms: Daily cleaning with hospital-grade disinfectants, especially in ICU and isolation wards.
- Floors and Corridors: Routine mopping and sanitization to prevent contamination spread.
Sterilization of Medical Equipment
Sterilizing reusable medical instruments is critical to prevent cross-contamination.
- Autoclaving: Uses high-pressure steam to sterilize surgical instruments.
- Chemical Sterilants: Used for heat-sensitive equipment like endoscopes.
- Single-Use Devices: Encouraged where feasible to reduce infection risks.
Waste Management
Proper disposal of medical and non-medical waste is essential to maintain hygiene.
- Segregation: Separate bins for infectious, sharps, pharmaceutical, and general waste.
- Sharps Disposal: Needle and blade disposal in puncture-resistant containers.
- Hazardous Waste Treatment: Incineration, chemical treatment, or autoclaving before disposal.
Air Quality and Ventilation
Clean air reduces the risk of airborne infections.
- HEPA Filters: Used in operating rooms and isolation units.
- Negative Pressure Rooms: Contain airborne pathogens in isolation wards.
- Regular Maintenance: Routine HVAC system checks to ensure air quality.
Best Practices for Maintaining Hospital Hygiene
Hospitals must adopt a comprehensive approach to maintain hygiene and sanitation effectively.
Implement Standard Operating Procedures (SOPs)
Clear SOPs guide staff on cleaning protocols, infection prevention, and waste management.
- Assign responsibilities for cleaning schedules.
- Specify disinfectants and concentration levels.
- Ensure compliance through routine audits.
Staff Training and Awareness
Continuous training ensures hospital staff adhere to hygiene standards.
- Infection control workshops and refresher courses.
- Demonstrations on proper handwashing, PPE use, and equipment sterilization.
- Encouraging reporting of breaches in hygiene practices.
Patient and Visitor Education
Educating patients and visitors supports hospital hygiene efforts.
- Signage on hand hygiene and respiratory etiquette.
- Instructions for safe disposal of used PPE or personal items.
- Awareness campaigns to prevent the spread of infections.
Infection Surveillance and Monitoring
Monitoring infection rates helps in timely intervention.
- Regular tracking of HAIs, surgical site infections, and outbreaks.
- Microbiological surveillance for high-risk areas.
- Immediate response plans for contamination events.
Use of Technology
Technology enhances hygiene and sanitation practices.
- Automated hand hygiene monitoring systems.
- UV light sterilization for rooms and equipment.
- Digital tracking of cleaning schedules and audits.
Emergency Preparedness
Hospitals must be ready to manage hygiene during outbreaks or disasters.
- Isolation protocols for infectious patients.
- Stockpiling of disinfectants, PPE, and sanitation supplies.
- Rapid training for staff on emergency hygiene protocols.
Common Challenges in Hospital Hygiene
Maintaining high hygiene standards is complex and requires addressing multiple challenges.
Staff Compliance
Inconsistent adherence to hygiene protocols can increase infection risks. Continuous monitoring and training are essential.
Resource Constraints
Limited budgets or shortages of disinfectants, PPE, and sterilization equipment can compromise hygiene practices.
High Patient Turnover
Busy hospitals with high patient volumes face challenges in maintaining consistent cleaning standards.
Emerging Pathogens
New infectious agents or drug-resistant bacteria require updated protocols and rapid adaptation.
Cross-Contamination
Movement of staff, equipment, and visitors between areas can spread pathogens if proper protocols are not followed.
Role of Hospital Administration in Hygiene
Hospital leadership plays a critical role in ensuring hygiene and sanitation.
- Policy Development: Establishing infection control policies and SOPs.
- Resource Allocation: Ensuring availability of cleaning supplies, PPE, and sterilization equipment.
- Monitoring and Evaluation: Conducting regular hygiene audits and inspections.
- Staff Support: Encouraging reporting of hygiene issues and rewarding compliance.
- Community Engagement: Promoting public awareness about hospital hygiene and infection prevention.
Impact of Hospital Hygiene on Patient Safety
Effective hygiene and sanitation directly influence patient outcomes.
- Reduced Infection Rates: Lower incidence of HAIs and surgical site infections.
- Shorter Hospital Stays: Patients recover faster in clean environments.
- Enhanced Patient Trust: Clean hospitals increase patient satisfaction and confidence.
- Lower Healthcare Costs: Preventing infections reduces treatment costs and resource utilization.
- Improved Staff Morale: Safe and hygienic workplaces enhance staff efficiency and well-being.
Conclusion
Hospital hygiene and sanitation are vital for ensuring patient safety, preventing infections, and promoting overall healthcare quality. By implementing rigorous protocols, training staff, monitoring compliance, and leveraging technology, hospitals can maintain high standards of cleanliness and minimize the risk of healthcare-associated infections. Awareness among patients, visitors, and staff further strengthens hygiene efforts, creating a safe and supportive healthcare environment. Maintaining hospital hygiene is not just a regulatory requirement but a core component of patient-centered care that protects lives and enhances healthcare outcomes.
FAQs
1. Why is hospital hygiene important for patient safety?
Hospital hygiene prevents infections, reduces complications, and ensures a safe environment for patients, staff, and visitors.
2. What are common hospital hygiene practices?
Hand hygiene, PPE use, environmental cleaning, sterilization of equipment, waste management, and air quality control are key practices.
3. How do hospitals prevent healthcare-associated infections (HAIs)?
Through strict cleaning protocols, proper sterilization, infection surveillance, staff training, and patient education.
4. Can technology improve hospital hygiene?
Yes, tools like automated hand hygiene monitoring, UV sterilization, and digital tracking of cleaning schedules enhance hygiene and compliance.
5. What role do patients and visitors play in hospital hygiene?
Patients and visitors help by following hand hygiene, using PPE as instructed, and adhering to infection control guidelines to prevent the spread of pathogens.